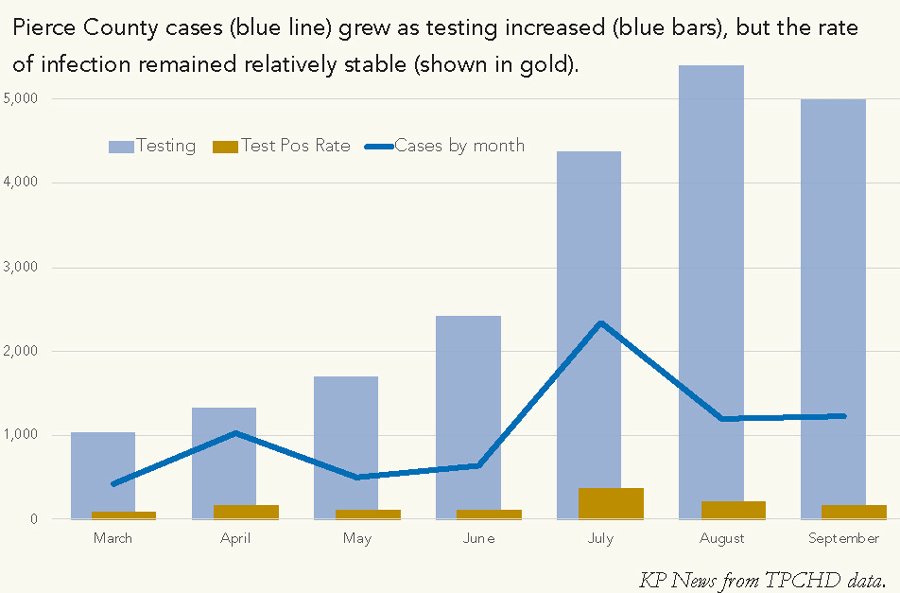
Pierce County is in Phase 2 of reopening, but advancing to the next phase has stalled as coronavirus infections have risen for the third time, according to the Tacoma-Pierce County Health Department. While increased testing has accounted for an increase in cases, the infection rate remained relatively steady at 3.9% (at press time).
Another wave of COVID-19 over the winter could be more severe than those of last spring and summer because it would coincide with other seasonal viruses like the flu, according to a September report from the Johns Hopkins University School of Medicine. More people could also be carrying the virus, causing it to spread more quickly.
More young people were infected recently in Pierce County than during the initial outbreak last spring: in mid-October, 21% of cases were in the 20-29 age group (13.6% of the county population) and 20.7% were in the 30-39 age group (13.4% of the population), higher than any other age group or infections in health care workers (10%). People of color have also been far more disproportionately affected, according to TPCHD.
Some experts attribute this shift to “pandemic fatigue,” where part of the population that does not consider COVID-19 a threat do not take precautions to prevent it.
“Right now, most people are still removed from the consequences of getting COVID-19,” wrote Carisa Parrish, co-director of pediatric medical psychology and an associate professor of psychiatry and behavioral sciences at Johns Hopkins in an August study.
“The risk might not feel real to them if they don’t know anyone who’s sick with COVID-19. And, unfortunately, some people get a bit of a thrill from doing something risky and escaping consequences,” she wrote.
According to Parrish and other experts, this increases the risk of a more deadly wave of the pandemic.
“Examples include the 1918 flu pandemic and the 2009 H1N1 flu epidemic. Both of these events began with a mild wave of infections in the spring, followed by another surge of cases in the fall,” a September report from Johns Hopkins said. “People are frustrated; cellphone data are showing decreased social distancing.”
President Donald Trump has expressed skepticism about the severity of the disease, even after having contracted it, and about public restrictions to curtail its spread, like mandates to wear masks his administration has quashed, according to the U.S. Centers for Disease Control and Prevention. Trump administration officials confirmed they began shifting coronavirus policies at the end of August from preventing its spread to focusing on the most vulnerable groups while pushing to reopen schools and businesses, according to reports in The Washington Post and The New York Times.
Dr. Anthony Fauci, director of the National Institute of Allergy and Infectious Diseases, told CNN on Sept. 21 that between 25% and 30% of the U.S. has a preexisting condition, like obesity, asthma or high blood pressure, that increases their risk of severe illness.
Approximately 20% of people who contract COVID-19 require hospitalization, according to the World Health Organization. By press time, at least 220,000 Americans had died from COVID-19, and as many as 75,000 remained ill with lingering effects, so-called “long hauler” patients, according to a peer-reviewed report in the Journal of the American Medical Association published in September.
What’s unusual about the long haulers, according to the JAMA report, is that many initially had mild to moderate symptoms that didn’t require lengthy hospitalizations.
The U.S. accounts for 20% of total global COVID-19 fatalities, the most recorded deaths of any country, while having just 4.25% of the global population. The true number of American COVID-19 deaths is thought to exceed official death counts already, according to a September analysis of unexplained deaths in excess of normal levels compiled by The New York Times. A September study from the CDC indicated that while seemingly less susceptible to it, children transmit the virus at a rate comparable to adults. The report said this doesn’t mean schools or day care facilities need to close, but that “masks, disinfection and social distancing are needed… People who work in such facilities have to be careful and get tested if they think they may be infected.”
Researchers from Utah and the CDC focused on three outbreaks in Salt Lake City child care facilities between April and July. They estimated the rate of spread at 25%, comparable to the spread in households with young children. Three of 12 infected children at one facility were asymptomatic, and one of them infected a parent who was later hospitalized.
In October, U.S. and Indian researchers published a study in the journal Science of 85,000 people with COVID-19 and 575,000 people they came in contact with, which found that children 17 and under contract and transmit the virus at rates similar to the rest of the population. Children age 5 to 17 passed the virus on to 18% of close contacts their same age. They also had the lowest death rate of any age cohort.
UNDERWRITTEN BY THE FUND FOR NONPROFIT NEWS (NEWSMATCH) AT THE MIAMI FOUNDATION, THE ANGEL GUILD, ADVERTISERS, DONORS AND PEOPLE WHO SUPPORT INDEPENDENT, NONPROFIT LOCAL NEWS